In 1978, leaders from across the world met in Alma-Ata, Kazakhstan, and affirmed the primary place of primary health care. Forty years after, they met again and reaffirmed the need for countries to fund PHCs adequately. In this concluding section of a two-part report, JUSTICE NWAFOR interrogates how years of Nigeria’s inadequate funding of NPHCDA (2012-2018) and the NCDC (2013-2018) left primary healthcare delivery and disease outbreak response ineffective. Read PART ONE here.
John Ezekiel, 32, wasn’t expecting a visitor at 4:55 pm. So, when this reporter walked into the hospital, his eyes darted from the reporter’s brown shoes to his dark hair, then to the pregnant woman seated next to him and back with a full gaze at the reporter. His demeanour was obvious and simple: ‘you shouldn’t have come now.’
However, his curious, hardened face gradually glowed and embraced some smiles when he realised the reporter wasn’t seeking any medical attention. Don’t blame John because a community health officer like him who sees electric bulbs lit in surrounding buildings but can’t have those in his hospital lit would always have his heart jump when a potential patient walks in at such time.
Well, it wouldn’t have been worse if there were enough funds to fuel the 1.5KVA petrol-powered generator packed at the back of the hospital. John wasn’t afraid to work, he would say, but really he was constrained because the conditions were not just right for him and the three nurses at Wumba Primary Health Centre (PHC) in Apo Resettlement Area — 10.5 miles from Aso Rock Presidential Villa, Abuja.
There is grid power supply in Wumba but the PHC is in darkness because the Abuja Municipal Area Council (AMAC) — which manages the hospital — is unable to pay the electricity bill of the hospital. Since February last year when Abuja Electricity Distribution Company (AEDC) — the firm which manages grid power supply in the city — disconnected the hospital due to a debt of about N110,000, generating off-grid power has cut really deep into the hospital’s meagre purse.
The cost of running the hospital’s power generator for a few hours in a day could be as much as N1,000, John told this reporter in October. Of course, the amount would have spiked with the latest increment in the petrol pump price in the country.
The cost wouldn’t have been much of a worry if the hospital got most of the consumables it needed from the government. “We buy drugs from the little money patients pay”, John said. Even when the city battled a surge of confirmed COVID-19 cases, nothing significant changed; Personal Protective Equipment (PPEs) were not supplied. “They didn’t give us even a hand sanitiser. The one here, I bought it. I was touching patients with bare hands. No hand gloves. There is no laboratory scientist,” he said.
Experts say most of the 30,000 PHCs in Nigeria do not meet the standard for functional PHCs all over the world. In fact, Nigeria’s immediate past Minister of Health, Isaac Adewole said only two in every 10 (20 per cent) primary healthcare facilities in the country were working.

Lagos: Not all glamorous
Abuja and Lagos have many beautiful things in common. Of course, the cities house embassies and consulates and the country’s busiest airports. While Lagos is Nigeria’s commercial hub, Abuja is its seat of power. But one site not so beautiful is the primary healthcare centre in Morning Star Street, Tiwadire, Ejigbo, Lagos. While Wumba PHC is up and running but lacks some facilities and supplies, the PHC at Morning Star Street has been abandoned for 16 years.
When this reporter visited the facility in October, it had been turned to a makeshift shelter for the homeless. The stench of urine and faeces was choky.
Unwashed plates and pots spluttered the entry to what was designed to be the reception hall. In all corners of the hall, torn insecticide treated nets hung above mats, some half folded. In rooms designed to be wards, loincloths, wrappers, shorts and shirts hung on nails fastened to the wall. And oil drips from packed motorcycles gave the grey-coloured floor tiles some dark stains.
Oludare Agboola, the Community Development Association (CDA) chairman of Tiwadire told Nigerian Tribune that the number of homeless riders in the abandoned facility which is designed to serve about 20 streets was over 200. “At night, you could count between 300 and 400 of them there. The abandoned facility is now a security threat.
“When politicians want to seek votes, they use it for campaigns and promise to complete the project if voted in. Even the Local Government Area (LGA) chairman made promises on it,” he said.

The Alma-Ata and Astana Declarations
In 1978, leaders from across the world met in Alma-Ata, Kazakhstan, and affirmed the primary place of PHC. The conference also agreed that “it forms an integral part of the country’s health system. It is the first level of contact of individuals, the family and community with the national health system bringing health care as close as possible to where people live and work, and constitutes the first element of a continuing health care process.”
This and a number of other statements were documented to form what has become known as the Alma-Ata Declaration.
Forty years later — in 2018 — Astana, Kazakhstan, global leaders met again and reaffirmed what was declared earlier. In clear terms, the conference stated that “strengthening primary health care is the most inclusive, effective and efficient approach to enhance people’s physical and mental health, as well as social well-being, and that PHC is a cornerstone of a sustainable health system for universal health coverage (UHC) and health-related Sustainable Development Goals”. This became part of the document that has become known as the Astana Declaration.
With the great intentions of the declarations, primary health care still wallows in neglect and endures inadequate funding, especially in Nigeria where its management lies with the local government system which has performed badly in recent years.
Revitalising community approach to solving healthcare needs — which is at the heart of primary health care — is, undoubtedly, one way Nigeria could scale up access to quality healthcare delivery and inch closer to realising the goals of universal health coverage, Dr Claire Standley, an Assistant Research Professor and Public Health Responses and Emergency Preparedness expert at the Center for Global Health Science and Security, Georgetown University, United States, told this reporter.
“Strengthening the foundation of the health system would help Nigeria to achieve to some extent the goals of the Universal Health Coverage and ensure that people have access to the basic services they require to help them live healthily and have fulfilling lives”, Dr Claire said.
Inadequate funding of the National Primary Health Care Development Agency (NPHCDA)
The NPHCDA was established in 1992. In 2007, it was merged with the National Programme on Immunisation. While the agency has been applauded for its role in eradicating polio from Nigeria, the same may not be totally said of its efforts in meeting its mandate in primary healthcare delivery, which include: making public health services available by ensuring communities have access to health facilities, services and basic health insurance.
Well, inadequate funding has been the bane of Nigeria’s health sector and NPHCDA is not an exception. What poor funding means is that the agency is unable to carry out its functions effectively, thereby making access to quality healthcare impossible.
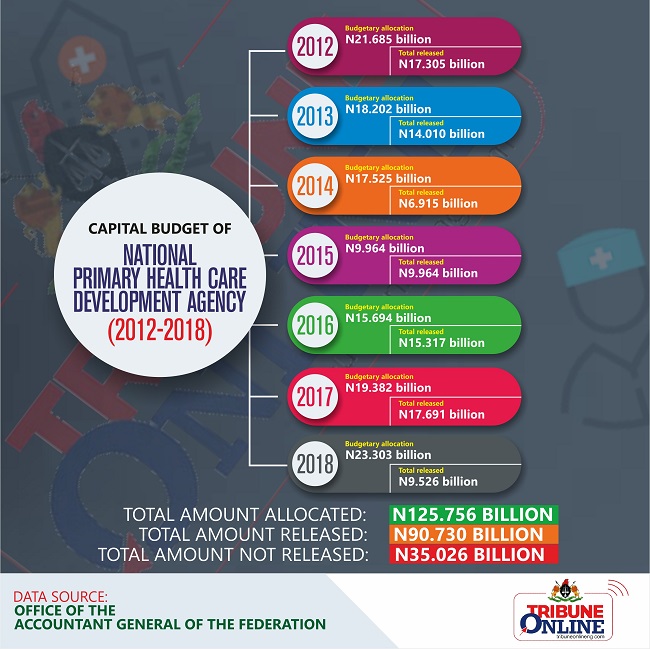
For the purpose of this report, Nigerian Tribune analysed the capital budgetary allocation of NPHCDA from 2012 to 2018 obtained from the office of the Accountant General of The Federation. Sadly, the analysis revealed that the highest allocation to the agency in the years under review was in 2018, N23.303 billion but less than half of the budgeted amount, N9.526 billion, was released to the agency. The incomplete release of budgeted funds wasn’t just for 2018. It was also witnessed in other years apart from 2015 when N9.964 billion was budgeted and the same was released.
The second highest allocation was in 2012 when N21.685 billion was budgeted but N17.305 billion was released. The next year, the budgeted amount went south to N18.202 billion while the total releases stayed somewhat stable at N14.010 billion. The southward trend continued in 2014; N17.525 billion was allocated and less than half of the amount, N6.915 billion was released.
The trend continued in 2016; N15.694 billion was released but the total releases improved remarkably — N15.317 billion. 2017 was significantly different as N19.382 billion was budgeted and N17.691 billion was released to the agency. For context, funds releases to Ministries, Departments and Agencies (MDAs) in Nigeria usually come in tranches and sometimes lack uniformity. For example, in 2018, the NPHCDA had its total releases come in two tranches: first was N4.330 billion and the second was N5.196 billion while in 2014 the releases came in three tranches. N1.933 billion (1,933,304,536) was first, N3.471 billion (3,471,586,849) second and N1.510 billion (1,510,292,422) third.

Further analysis revealed that from 2012 to 2018, a total of N125.756 billion was allocated to the NPHCDA for capital expenditure but only N90.730 billion was released. This means N35.026 billion was not released to the agency. This wouldn’t have been a huge cause for concern if health outcome indices of Nigeria weren’t so dire and if the sector had been receiving adequate funding in the recent past.
If the withheld funds were actually released and utilised properly, it should have helped better healthcare delivery in the country. To better understand the impact of this, Nigerian Tribune estimated the facilities it should have provided in far-flung communities in the country.
Nigerian Tribune obtained procurement data from Budeshi — one of Nigeria’s leading platforms for budget and procurement data. Owing to the fact that this report examines budget data from 2012 to 2018, a project awarded in 2016 by NPHCDA — the construction of a PHC (type one) at Ung. Waziri in Kudan LGA of Kaduna State — was used to estimate how much it would cost to establish a similar project during that period. The project was budgeted to cost N28 million.
At the budget amount of N28 million for a type one PHC, the N35.026 billion (N35,026,089,892) could have been enough to erect approximately 1,251 type one PHCs. Of this number, each of Nigeria’s 36 states and Abuja could has got 33. It means each of the country’s 774 Local Government Areas (LGAs) should have gotten at least one.

No doubt, funding of critical health institutions like the NPHCDA has to improve if Nigeria wishes to achieve UHC. But there is more to funding, Dr Claire thinks. She says it’s time to go beyond allocating and releasing funds alone. The released funds should be monitored closely to ensure they are utilised solely for what they were budgeted for. “You need to make judgments based on cultural contexts and local needs. Find out where we need to invest to create the level of health system we want,” she advised.
Brain drain: ‘Leaving Nigeria is inevitable’
There’s more to the health sector’s inadequate funding than poor facilities at the hospitals and lack of quality healthcare services — the country loses its best brains to countries with better conditions of work. In 2018, Adewole said Nigeria had only one doctor per 5,000 people against the recommendation of one doctor per 600 population.
In the same year, the Medical and Dental Council of Nigeria (MDCN) said there were about 72,000 nationally-registered Nigerian doctors, with only 35,000 practising in the country as of 2018. When this figure is factored with the national population estimate of 200 million, it leaves a deficit of over 260,000 doctors in Nigeria. This means that a minimum of 10,400 new doctors need to be recruited annually for 25 consecutive years to meet the target.
The gap may be closed substantially if the 3000 medical doctors trained annually in the country, of which about 2000 leave, stay back and practise. But, Chairman of the country’s union of medical doctors — Nigeria Medical Association (NMA) — Oyo State branch, Dr Akin Sodipo told Nigerian Tribune, earlier in the year, it’s a tall dream. “You cannot force a doctor to stay back in the country and practise amidst poor infrastructure and other debilitating challenges,” he said.
Dr Mayowa Adeyemi, the doctor at Samuel Adegbite Memorial Hospital, Igbo-Oloyin, couldn’t have said it better: “I’m still in Nigeria because it’s not yet time for me to leave. But leaving is inevitable.”
Dr Adeyemi wouldn’t be the first to leave. In fact, there are 8,009 doctors who qualified in Nigeria practising in the UK as of November 23, 2020, according to data from the UK General Medical Council register. And the UK is just one of the many choice locations for Nigeria trained doctors.
Doctors are not the only ones leaving. Nigeria’s elite, including the country’s current and past presidents, governors of states, lawmakers and cabinet ministers jet out of the country to get quality medical care. This, the Nigerian Sovereign Investment Authority (NSIA) says, costs the country $1 billion annually — an amount way bigger than its seven years (2012-2018) health sector capital budget.

Nigeria Centre for Disease Control (NCDC): In the eye of the storm
The Nigeria Centre for Disease Control is Nigeria’s elite health institution charged with the mandate to lead the preparedness, detection and response to infectious disease outbreaks and public health emergencies. The agency was applauded for its role in managing the Ebola Virus Disease outbreak which the agency’s Director General (DG), Dr Chikwe Ihekweazu described in 2018 as the young agency’s first experience in leading the response to a major outbreak. He warned that the preparedness and response capacity of countries (like Nigeria) requires significant investments to strengthen their health systems.
Analysis of the agency’s capital budget from 2013 to 2018 obtained from the office of Nigeria’s accountant general showed that as in NPHCDA, NCDC got its highest capital budgetary allocation among the years under review in 2018, N1.635 billion but not up to 40 per cent of that amount, N654.241 million was released.
2015 was the worst year both in the total amount allocated and the amount released: N224 million and N112 million. In 2013, N841.541 million was budgeted but N500.655 million was released. It went drastically lower the next year with N355.846 million budget for the agency, but less than half of the amount was released, N145.789 million. N248.507 million was budgeted for it in 2016 but N155.074 million was released. The figures went encouragingly high in 2017 to N1.565 billion. The same year witnessed the highest releases among the years reviewed: N782.551 billion.
Nigerian Tribune analysis showed that in six years (2013 to 2018), the Federal Government of Nigeria allocated N4.870 billion for capital development of its elite disease control agency. Of this amount, less than half was released: N2.350 billion. Sadly, more than half was not released: N2.520 billion.
Dr Ihekweazu told Nigerian Tribune that “it is incorrect to say that we were unprepared; prior to the first confirmed case in Nigeria, we had set up testing capacity at the NCDC National Reference Laboratory and two other laboratories within our network of public health laboratories”. But he admitted that “we could have been better prepared when COVID-19 came.”
He explained that “the Government of Nigeria has provided rapid funding in response to the COVID-19 pandemic. Through this, we have been able to scale up on various activities that we began prior to this outbreak.”
The response could have been better if the agency was adequately funded, perhaps, if the budgeted funds were totally released, to say the least. “There are several areas that we could have been better prepared if early investments were made. For example, it was evident that even though we had five molecular laboratories for Lassa Fever, they were grossly insufficient for a pandemic the scale of COVID-19. So, appropriate funding could have enabled us to build our capacity earlier than we did”, Dr Ihekweazu said.
No response
Nigerian Tribune contacted the Lagos State Commissioner for Health, Professor Akin Abayomi for a conversation around its findings. He demanded questions be sent to him via email. They were sent several times but Abayomi is yet to respond as at the time of filing this report.
Ganiyu Johnson represents Oshodi-Isolo II Federal Constituency, in which Tiwadire is, at Nigeria’s House of Representatives. Nigerian Tribune called the mobile number displayed on his profile on the website of the National Assembly but got no response.
Monsuru Obe, the Chairman of Ejigbo Local Council Development Area, in which Tiwadire is, was also contacted by Nigerian Tribune but he declined to comment.
However, when the Lagos State government mooted the idea of asking COVID-19 patients with mild symptoms to isolate at PHCs, not many saw it working because of conditions like that of Tiwadire PHC. But Professor Abayomi, in a July report, said innovative measures were being employed to curb the explosion of cases including the management of cases electronically.
“We manage asymptomatic or mild cases of coronavirus electronically. We keep in touch through telephone, telemedicine, zoom calls, and other ways of monitoring people who are self-isolating at home, including home visits if possible,” he said.
This work was produced as a result of a grant provided by the Africa-China Reporting Project at the Journalism Department of the University of the Witwatersrand. The opinions expressed and conclusions drawn are the author’s own and do not represent those of the project.



